For people 2 years of age and older with active psoriatic arthritis

PSORIATIC ARTHRITIS FACTS AND SYMPTOMS
What causes psoriatic arthritis?
Psoriatic arthritis (PsA) is an inflammatory, autoimmune condition that can affect both the joints and skin. The specific cause of psoriatic arthritis is not fully known, though it’s believed that an overproduction of molecules in your body may activate any of the multiple symptoms of PsA.
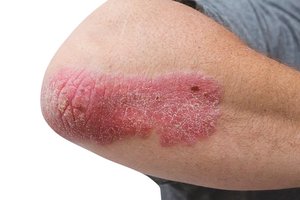
When these molecules, such as the IL-17A protein, are overproduced, your body’s immune system has inflammatory responses that can contribute to pain and swelling in the joints and tendons, and sometimes, even skin plaques—raised patches of red skin that are thick, scaly, and itchy.
Without proper treatment, PsA may worsen, which is also known as psoriatic arthritis flares. And if left untreated, psoriatic arthritis may cause permanent joint damage.
Psoriatic arthritis (PsA) isn’t caused from overuse of joints or aging. It’s the result of an overactive immune system.
What are the first signs of psoriatic arthritis?
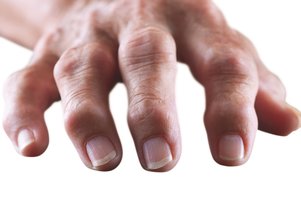
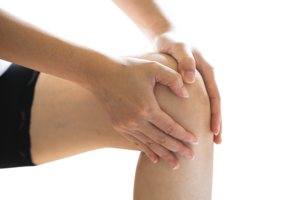
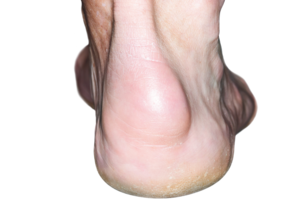
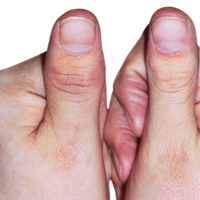
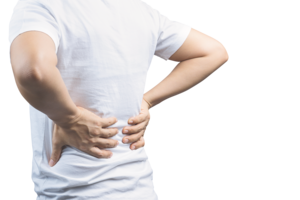
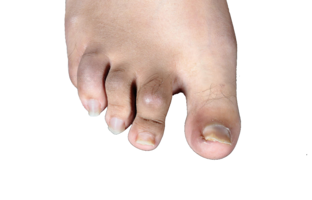
The first signs of psoriatic arthritis are not the same for everyone and can affect each person differently. PsA symptoms can include:

Men and women are equally at risk of developing PsA
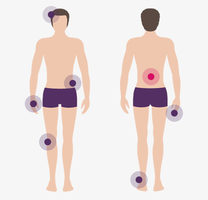
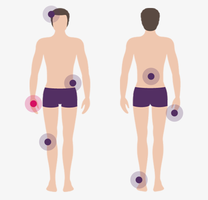
What are the symptoms of psoriatic arthritis?
There are multiple symptoms of psoriatic arthritis, like joint pain and fatigue. These symptoms affect everyone differently. Use the sliders below the images to learn more about these symptoms and how they can affect you.
Quotes from actual patients who were compensated for their time.
FIND A DOCTOR
Ask your rheumatologist if COSENTYX® may be right for you.
Real people taking COSENTYX are looking and feeling better. Could you be one of them?
Individual results may vary. Jorge and Tina were compensated for their time.